We are living in a generation of advancement where women are empowered with multiple alternatives to secured birth control. Right from the beginning of traditional birth control methods such as hormonal pills to long-acting reversible contraceptives (LARCs) like intrauterine devices (IUDs), important scientific advancements and technological innovations have reshaped the landscape of women's reproductive health and birth control. Genetic research has also played a role in developing more tailored contraceptive solutions, addressing individual variations in drug response. Overall, these advancements have empowered women with a wider array of choices, ensuring improved family planning outcomes.
While each option has its own set of pros and cons. Intrauterine Devices (IUDs) are one such popular alternative, tiny, t-shaped plastic or copper contraceptive devices employed in the uterus for extensive contraception. Owing to its effectiveness and convenience, they have emerged in marketability. So let us dive deep into the attributes of IUDs in this blog, magnifying multiple varieties, usefulness, and possible adverse effects.
In order to prevent unwanted pregnancy, an IUD is employed in a woman's uterus. It is a form of contraception that has two variables namely, Hormonal and Copper Bearing IUDs. Both have their unique operation and are meant to prevent pregnancies. They are about a size of a quarter and need no daily care, making a good birth control option for women of child bearing age group, showcasing that age is not a barrier for IUD use.
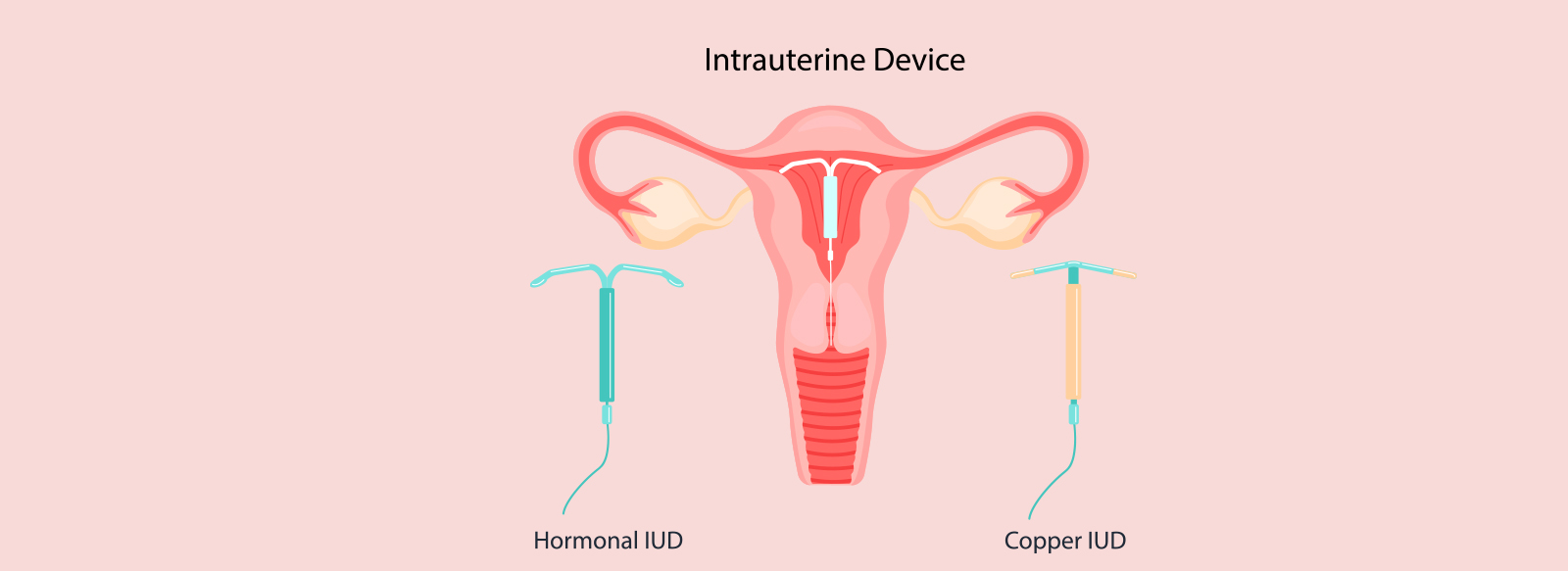
There are two main types of IUDs: Hormonal IUDs and Copper Bearing IUDs.
Hormonal IUD: The hormone progestin is released into the uterus by this type of IUD. The progestin thickens the cervical mucus, making sperm harder to reach the egg. Furthermore, it has an effect on the uterine lining, making it less susceptible to a fertilised egg.
Copper Bearing IUD: The IUD works by preventing fertilization. The Copper Bearing IUD releases copper ions into the uterine cavity which are toxic to the sperm entering the uterus and fallopian tubes. IUDs affect the endometrial lining and may prevent implantation of a fertilized egg. However, the primary mechanism of action for the IUD is to prevent fertility earlier in the reproduction process before the egg reaches the uterus.
One of the primary reasons IUDs are becoming more popular is their extraordinary efficiency. They are among the most dependable birth control methods available. IUDs are frequently likened to sterilisation in terms of efficacy but with the considerable benefit of reversibility. IUDs have a shallow pregnancy rate, less than 1%, making them practically as successful as permanent sterilisation treatments.
Thickening Cervical Mucus: Hormonal IUDs releases a hormone called progestin which hardens cervical mucus, prohibiting the sperm from getting via the cervix and reaching the uterus.
Fertilisation Suppression: In very few cases, the hormone progestin stops the release of eggs from the ovaries, slowing down the ovulation process. So, it becomes impossible to ensure pregnancy without a viable egg.
Changing the Uterine Lining: The Hormonal IUD creates a barrier in the uterine lining, making it lesser or not at all responsive to a fertilized egg. It reduces the chances of the egg implanting in the uterus, making the sperm incapable of the results.
Sperm toxicity: Copper ions released by the Copper Bearing IUD poison sperm, destroying or immobilising them. This inhibits fertilisation from occurring.
Inducing an Inflammatory Reaction: Since the copper causes an inflammatory response in the uterus, it leads to the sperm's failure to make it to the egg.
The procedure for inserting an IUD is straightforward. During a brief clinic visit , a healthcare professional implants the device into the uterus. This technique is usually painless. Following insertion, a thin thread extends down into the vaginal canal, allowing the user to ensure that the IUD is securely in place.
IUD removal is also a simple procedure which has to be performed by a healthcare professional. It entails carefully removing the IUD out of the cervix. Fertility normally returns to normal within few weeks when the procedure is completed. IUDs are convenient since they are long-acting and can give protection for several years, depending on the kind and brand.
It is important to emphasize the efficiency of IUDs in preventing pregnancy. IUDs, as previously stated, are extremely successful, with a failure rate of less than 1%. As a result, they are more dependable than many other contraceptive techniques. The fundamental reason for their remarkable effectiveness is that there is no space for human mistakes once they are installed. The effectiveness of measures such as birth control tablets or condoms might be jeopardised if they are not used regularly and appropriately. This is no longer an issue with IUDs.
If put within a certain interval following unprotected intercourse, IUDs can also be used as emergency contraception. WHO recommends that a copper-bearing IUD, when used as an emergency contraceptive method, be inserted within 5 days of unprotected intercourse. Contraception in an emergency IUDs primarily function by preventing the fertilised egg from implanting in the uterus. This highlights their adaptability and the fact that they may be used as both long-term and emergency contraceptives.
While IUDs are known to be extremely effective, each coin has two sides. Thus, when choosing an IUD, it is vital to know the negative effects it can possibly cause.
Pain and Discomfort: Some women report discomfort or pain during and after IUD implantation. This is generally just transitory and is treated with some pain relieving medicines.
Irregular Menstrual Bleeding: Menstrual cycle irregularities are a typical adverse effect of Hormonal IUDs. This might appear as lighter or heavier periods, spotting between periods, or, in extreme circumstances, the lack of periods. Copper Bearing IUDs, on the other hand, may cause heavier and more painful periods.
Expulsion: The IUD may be expelled from the uterus in rare situations, particularly in the first few months following placement. It can happen without the wearer recognising, thus checking the IUD string on a regular basis is critical and important.
Infection and Pelvic Inflammatory Disease (PID): Although there are minor chances, infection during IUD placement is quite possible, leading to PID. It is a disorder resulting in pelvic discomfort and infertility, if not treated on time.
Ectopic Fertility: IUDs are great at eliminating intrauterine pregnancies. But if it occurs while wearing an IUD, there are chances of an ectopic pregnancy that implants the fertilized egg outside the uterus.
Reactions to Allergens: In rare cases, women may have an allergic reaction to the materials in an IUD.
Both the forms of IUDs i.e. Hormonal & Copper Bearing are effective birth control methods as they prohibit the fertilization process. Apart from being dependable, they are also completely reversible. They provide Contraception for up to 3-10 years. With such great advantages, they surpass all the rare side effects. So, consult with a healthcare expert and get the best option for you that suits your individual requirements and preferences.
